A rare, pyogenic, granulomatous, subacute to chronic infection caused by actinomycetes. Actinomycetes are a group of anaerobic gram-positive bacteria with high guanine-cytosine content found as natural flora of the oral cavity.
The most frequent features are ulcer and granuloma formation, and the presence of multiple abscesses and sinus tracts that may discharge sulfur granules. The pathogens often spread into neighbouring tissues.
Actinomycetes often invade the body by microfissures, and the most common clinical form of actinomycosis is cervicofacial, either after oral surgery or caused by poor dental hygiene.
Thoracic and abdominal actinomycoses also occur frequently, and pelvic actinomycosis is possible in women.
Prolonged antibiotic treatment is necessary.
Whipple's disease, which may be interpreted as a special form of actinomycosis, since it is caused by Tropheryma whipplei, a pathogen from the clade of actinomycetes, is not discussed here.
The incidence of actinomycosis was about 1/300,000 per year in the 1970s. This seems to have decreased, owing to improved dental hygiene and the widespread use of antibiotic treatment.
The disease is becoming rarer in industrialised countries, although it might be more common in developing countries that have lower hygiene standards.
There is no predilection for age, race, season, or occupation. However, there seems to be a male-to-female ratio of between 1.5:1 and 3:1.
Aetiology
Actinomycosis is caused by branching gram-positive bacteria. Actinomycosis was first described in 1878 and first isolated under anaerobic conditions in 1891.
Actinomyces are strict or facultative anaerobes.
The bacteria form diphtheroidal or coccoidal filaments and resemble fungi.
They are part of the normal intestinal and oral flora and are particularly located in periodontal pockets, dental plaque, and dental caries.
The main species involved in human disease is Actinomyces israelii. However, more than 30 species have been linked to human disease.
Actinomyces are almost invariably isolated as part of a polymicrobial flora. However, the significance of these co-isolated bacteria in the pathogenesis of actinomycosis remains unclear.
Pathophysiology
Because actinomycosis is an infection with various manifestations, clinical features vary. Actinomycetes acquire pathogenicity through invasion of breached or necrotic tissue. Once infection is established, the host mounts an intense inflammatory response (i.e., with suppuration and granuloma formation).
Fibrosis may then follow. Infection typically spreads contiguously and invades surrounding tissues or organs. Ultimately, the infection produces draining sinus tracts, which are a hallmark of the infection.
Infections are seen most commonly in the cervicofacial area (50% to 70%), followed by the abdomen (10% to 20%).
Other manifestations, such as thoracic or CNS actinomycosis, are much rarer and are found only as sporadic case reports.
Cervicofacial actinomycosis often starts after a tissue injury or orofaciomaxillary trauma. In its initial stages it is characterised by soft-tissue swelling of the perimandibular area.
Spread occurs over time into adjacent tissues.
As a consequence of infection, fistulae (sinus tracts) develop, and these discharge purulent material containing granules with a yellow sulfur-like appearance (termed sulfur granules).
Invasion of the cranium or the bloodstream is seen very rarely, but may occur if the disease is misdiagnosed or left untreated.
Actinomycosis frequently follows surgery. The disease tends to spread locally in a contiguous fashion, disregarding tissue borders.
Lymphadenopathy is not typical, and haematogenous dissemination is rare.
Because of the slow growth of the pathogen, disease may develop over months to years before diagnosis is made.
Classification
Taxonomic classification
Actinomycetes are a group of gram-positive bacteria with high guanine-cytosine content.
Most actinomycetes of medical or economic significance are in the subclass Actinobacteridae, order Actinomycetales.
Although many of these cause disease in humans, Streptomyces is notable as a source of antibiotics.
↚
Approach to diagnosis of Actinomycosis
Typically, actinomycosis presents as a chronic, slowly progressive, indurated mass. Clinical symptoms may be very subtle. Pain, fever, and fatigue, though sometimes present, are often absent. Characteristic lesions usually develop slowly, over weeks to months.
Actinomycosis has often been called the 'great pretender' or the 'great masquerader' of head and neck diseases, reflecting the fact that the symptoms are not specific and may be found in other, much more common conditions.
Thus, the inclusion of actinomycosis in the differential diagnosis of other possible diseases is often the only means to an early and correct diagnosis.
Actinomycosis is usually diagnosed only after surgery for treatment of an abscess or tumour. Only rarely is the diagnosis made before surgery.
Macroscopic and histological analyses of the pus from draining sinuses and detection of sulfur granules are highly indicative of actinomycosis, and may be confirmed by cultivation of actinomycetes.
Actinomycosis is more common in patients with diabetes mellitus and in those who are malnourished or immunosuppressed. It often develops in tissues that have been damaged by neoplasia, trauma, or irradiation.
It is more common in males than females, in a ratio of between 1.5:1 and 3:1.
Cervicofacial actinomycosis
Most cases of cervicofacial actinomycosis are odontogenic, and often result from injury or inflammation in the oral cavity.
However, primary infections have also been reported from other structures within the head and neck, sometimes anatomically significantly removed from any potential periodontal source.
Typically, cervicofacial actinomycosis presents as a chronic, slowly progressive, indurated mass, which develops into multiple abscesses, fistulae, and draining sinus tracts.
The visible inflammation is often more severe than the pain.
The involved skin may appear bluish or reddish.
Over time, sinus tracts and fistulae develop on the skin or mucosa, which may erupt and express a thick, yellow serous exudate containing so-called sulfur granules, which can sometimes be seen with the naked eye.
Cervicofacial actinomycosis may involve almost any tissue or structure surrounding the upper or lower mandible, and the mandible itself is often involved during infection. Fistulisation from the perimandibular region may be a first diagnostic clue.
Chewing may be difficult if the muscles of mastication are involved. A mass may be visible on CT or MRI, but this is unlikely to be diagnostic.
In a relatively large series of 317 patients, the presenting sites were:
- Mandible (54%)
- Cheek (16%)
- Chin (13%)
- Submaxillary ramus and angle (11%)
- Upper jaw (6%).
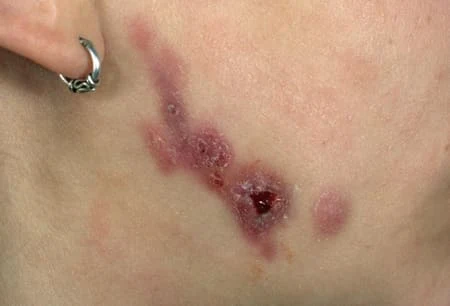 |
| Example of the clinical picture of a cervicofacial actinomycosis |
Abdominal and pelvic actinomycosis
Between 10% and 20% of all reported cases of actinomycosis are located in the abdomen or pelvis.
Typically, these patients have a history of tissue injury caused by recent or remote bowel surgery or ingestion of foreign bodies, during which actinomycetes were able to enter the deep tissues.
The infection typically presents as a slowly growing mass, and most frequently involves the ileocaecal region.
The mass may be visible on imaging studies such as MRI or CT, but the diagnosis is usually established only after exploratory laparotomy, by histology.
Intestinal actinomycosis may be misdiagnosed as Crohn's disease, malignancy, or intestinal tuberculosis. Any abdominal organ, including the abdominal wall, can be involved by direct spread, with eventual formation of draining sinuses.
Symptoms are often non-specific, and may include anorexia, nausea, vomiting, and abdominal discomfort. Some patients report the sensation of a mass in the abdomen.
Pelvic actinomycosis most commonly ascends from the uterus, and is usually caused by IUDs that have been in situ and not replaced for many years.
Patients may present with vaginal discharge or bleeding. Lower abdominal discomfort is also sometimes reported. Physical findings may include a palpable mass, visible sinus tracts, or fistulae.
Other manifestations
Thoracic actinomycosis is frequently misdiagnosed as malignant disease.
Actinomycosis may develop at any site in the chest, but it is most common at sites where the mucosal surface is altered or at sites of previous injury.
Aspiration, as occurs in conditions such as dementia or alcoholism, enhances the risk of pulmonary actinomycosis.
Symptoms referable to the chest are usually non-specific, and are determined by the location and the local extension.
They may include a cough, which can be dry or productive of sputum that may be blood-streaked; shortness of breath; and chest pain. Most patients present with local tumours visualised by radiological procedures.
In pulmonary actinomycosis, sinus tracts with sulfur granules may appear and are a strong diagnostic hint.
Actinomycosis may affect any organ or body system, including the CNS, presenting in most cases as brain abscess and rarely as meningitis or meningoencephalitis, actinomycoma, subdural empyema, or epidural abscess.
Other locations may be the skin, eye, or soft tissues.
Laboratory tests
Because actinomycosis is rare, and symptoms and physical findings, as well as laboratory results, are non-specific, diagnosis is usually made late in the course of the disease.
FBC may show anaemia and leukocytosis.
Even in specialist clinics, the time from first symptoms to diagnosis is frequently longer than 6 months.
The cornerstones of definitive diagnosis are:
- Direct cultivation of the agent from affected tissue
- Histology and immunohistology.
Culture
Actinomycosis is usually diagnosed by culturing the pathogen from affected tissue.
Typically, needle aspirates from an abscess, fistula, or sinus tract are used, although sometimes larger biopsy specimens are required.
Care should be taken to avoid contamination with other bacteria. Specimens should be incubated under strict anaerobic or at least microaerophilic conditions.
Culture requires a minimum of 14 days. Thus, culture techniques need to be meticulous and long incubation is required. False-negative results are not uncommon.
Moreover, patients have often already been treated with antibiotics before the differential diagnosis of actinomycosis is considered. In such cases, culturing the agent is difficult or impossible.
Therefore, although culture of the organism from affected tissue is the preferred diagnostic test, in many cases the diagnosis can be made only by histology or immunohistology.
↚
Histology and immunohistology
Biopsies from the affected tissue should be used not only for culture but also for additional histological work-up. Sections from biopsies reveal acute or chronic inflammation and granulation. Neutrophils, foamy macrophages, plasma cells, and lymphocytes surrounding dense fibrotic tissue are usually found.
A hallmark of actinomycosis is the presence of so-called sulfur granules, which are formed by the actinomycetes within the infected tissue.
This term may be misleading, because the granules do not contain sulfur. Rather, the name reflects the yellow colour of the granule in pus. Sulfur granules may be seen in only a few sections and in low density, and sometimes more than 1 biopsy is needed to confirm the diagnosis by this method.
The granules are often discrete, about 100 to 1000 micrometres in diameter, and are often seen directly without magnification or under the microscope with low magnification.
The granules are composed of a protein-polysaccharide complex and are mineralised by host calcium and phosphate.
The appearance has been described as internal mycelial fragments surrounded by a rosette of peripheral clubs.
Although these granules are typical for actinomycosis, similar granules may also be found in infections with other organisms (e.g., Nocardia brasiliensis or Streptomyces madurae), although the granules of bacteria other than actinomycetes usually lack the peripheral clubs.
Classifying the causative micro-organism solely by non-specific histological staining (haematoxylin and eosin, Gram, Ziehl-Neelsen, periodic acid-Schiff) is not possible.
Immunohistological techniques using species-specific staining with fluorescent-conjugated monoclonal antibodies have improved diagnostic procedures.
They identify the infecting actinomycete species reliably, and allow discrimination from other bacteria.
 |
| Periodic acid-Schiff stain of a mass of actinomycetes in a lymph node |
Other laboratory techniques
Other approaches have been used to try to improve the diagnostic tools for actinomycosis.
PCR techniques have been developed for the various species of actinomycetes. However, no standardised protocols exist.
PCR is used mainly in research studies, and has not yet become part of routine diagnostic practice. Serology has so far not improved the diagnosis of actinomycosis.
↚
Treatment approach
Actinomycosis is usually diagnosed after surgery for treatment of an abscess or tumour. High-dose, prolonged systemic antibiotic treatment is necessary, sometimes in combination with surgery.
With this approach, the outcome is favourable in more than 90% of cases. Relapse is rare after sufficient antibiotic treatment. If it occurs, it is treated in the same way as a primary infection.
Management and antibiotic treatment
High-dose penicillin is the preferred choice, given intravenously for 4 to 6 weeks, followed by oral therapy for a further 3 to 6 months.
Intravenous therapy can be given on an inpatient or outpatient basis, depending on the severity of disease.
For patients who are allergic to penicillin, parenteral ceftriaxone, clindamycin, erythromycin, or doxycycline can be used.
Patients with mild cervicofacial actinomycosis of endodontic origin may be given oral doxycycline from the outset.
Excision of lesions
Surgery should be reserved for excision of lesions in patients with extensive lesions, extensive necrosis, or large abscess formation.
Sometimes persistent fistulae must be removed by surgery. In patients in whom a malignant process cannot be ruled out, surgery may also be necessary for final diagnosis and treatment planning.
Treatment algorithm
Please note that formulations/routes and doses may differ between drug names and brands, drug formularies, or locations. Treatment recommendations are specific to patient group.
1st line
penicillin or amoxicillin
with extensive lesions, extensive necrosis, large abscess formation, and/or persistent fistula.
Plus:
surgical excision of lesions
Treatment recommended for ALL patients in selected patient group
These patients may require surgery to excise the lesions, in addition to antibiotics.
Penicillin allergic patients
1st line:
non-penicillin antibiotics
Ceftriaxone, clindamycin, erythromycin, or doxycycline can be used. Therapy needs to be given for several months. Most regimens involve an initial period of parenteral therapy, which can be given on an inpatient or outpatient basis, depending on severity of disease.
Patients with mild cervicofacial actinomycosis of endodontic origin may be given oral doxycycline from the outset.
For example:
ceftriaxone: 2 g intravenously/intramuscularly every 12-24 hours for 4-6 weeks.
and:
doxycycline: 100 mg orally twice daily for 3-6 months after cessation of intravenous therapy.
