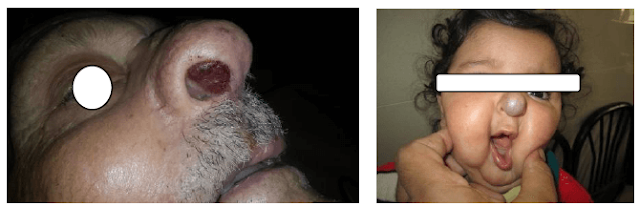
Benign sino-nasal tumors are abnormal groths that do not spread nor invade other parts of the body and they are not life threatening. They are non-cancerous but they are usually surgically removed for prevention and they have recurrence rate as cancerous tumours.
Classification and types:
Benign Tumors of the Nose and Paranasal Sinuses are classified into:
a. Epithelial
- Papilloma.
- Adenoma.
b. Non-epithelial
- Hemangioma.
- Osteoma.
- Fibro-osseous lesions.
- Chondroma.
- Neurolemmoma.
Detailed review of Common Benign Tumors
1. Osteoma
Pathology:
Types:
- Compact (Ivory) osteoma: common in frontal sinus.
- Cancellous (spongy) osteoma: common in ethmoidal sinus.
Site: It occurs in junction areas between membranous and cartilaginous bone where remnants of embryonal periosteum persist.
Incidence
- It is commoner in females than in males.
- It is common in Middle East area.
Association: multiple osteomata may be associated with intestinal polyposis (Gardner syndrome).
Symptoms:
- Asymptomatic in most of the cases (discovered accidentally).
- Painless slowly growing swelling.
- Manifestations of pressure and encroachment on the surrounding structures e.g. headache, proptosis, mucocele, nasal obstruction, deterioration of vision.
Signs:
- Hard, well defined swelling.
- May be seen in the nose.
Investigations: Plain X ray -C.T.
Treatment:
- Surgical excision if symptomatizing.
- This can be done either externally, or endoscopically.
2. Fibrous dysplasia
Definition: It is not a real tumor. It is an obscure bone disease where normal osseous tissue is absorbed and replaced by fibrous tissue and poorly formed bone trabeculae.
Etiology: Unknown, may be developmental.
Incidence:
- 2.5% of all bony neoplasm.
- Common in the 1st and 2nd decades.
- Common in females.
Pathology:
According to the affected sites, it may be:
- Monostotic: single site. In the head and neck, the maxilla is the commonest site.
- Polystotic: several sites including long bones, mostly unilateral .It may be associated with cutaneous pigmentation and endocrinal disturbance as precocious puberty, diabetes mellitus or hyperthyroidism (Albright syndrome).
- The growth tends to slow down after puberty and stops after complete osseous maturity.
- It does not turn malignant except if irradiated.
- Histologically, there is a mixture of fibrous and osseous tissue.
Symptoms:
Painless slowly growing swelling mostly in the maxilla and alveolar process causing:
- Disfigurement.
- Loosening of teeth.
- Nasal obstruction.
- Proptosis.
- Facial pain and numbness due to involvement of infraorbital foramen.
Signs:
- Diffuse, ill defined, non-tender, hard bony swelling.
Investigations:
- X-ray: hyperdensity of the facial bones with ground glass appearance.
- Increased serum alkaline phosphatase.
- Radioactive bone scan will show an increased uptake in all the affected sites.
Treatment:
- As the lesion tends to stabilize after puberty, no treatment is indicated unless there are manifestations.
- Limited trimming is indicated if the mass is disfiguring or causing pressure manifestations.
4. Hemangioma
Clinico-pathological types:
a. Capillary hemangioma (Bleeding polypus of septum).
- It presents as a soft red blue polyp on the nasal septum causing epistaxis.
- Treatment is by surgical excision with cauterization of the base. Laser may be used.
b. Cavernous hemangioma:
- Commoner in children.
- It arises from the lateral nasal wall especially the area of the inferior and middle turbinates. I
- t causes epistaxis and sometimes nasal obstruction if large.
- Treatment is by excision either surgically, by laser or by cryo-surgery.
- Congenital vascular malformation of hereditary origin.
- It runs in families. It may involve the nose, lips, face, oral mucosa, palate, tongue, pharynx and larynx.
- It causes recurrent epistaxis.
- It is treated by laser or surgical excision of the affected nasal mucous membrane.