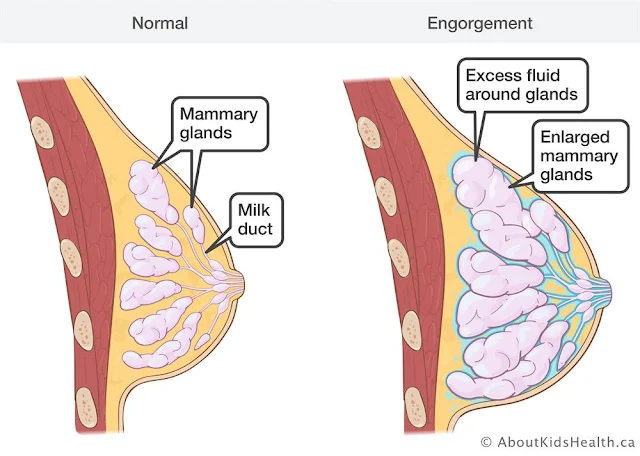
Definition: Acute bacterial inflammation of the breast which occurs during lactation.
Incidence: Most common type of mastitis.
Etiology
Causative Organism: Staph. aureus (coagulase positive).
The organism causes clotting of milk.
Route of infection:
- Direct spread (Main route) ) from mouth of suckling infant through nipple cracks & opening of lactiferous duct.
- Blood spread (less common) from a septic focus.
Predisposing Factors:
- Milk engorgement due to blockage of ducts by inspissated milk & epithelial debris.
- Nipple cracks & fissures caused by suckling . Retracted nipple is more likely to be injured by the baby (who tries to get hold of it).
- Bad hygiene.
- Bad general condition as diabetes, steroid therapy.
Pathology:
- At first, infection is usually diffuse.
- Milk engorgement >> not treated well >> acute mastitis >> necrosis by staphylococci >> multilocular abscess.
Clinical Picture
The clinical picture of Lactational Mastitis includes the following stages:
1. Stage of Milk engorgement
Symptoms:
- Dull aching pain.
- Mild persistent pyrexia.
Signs:
Enlargement & induration of the breast with no signs of inflammation.
2. Stage of Cellulitis (Mastitis)
Symptoms:
- The pain worsens
- Continuous high pyrexia
Signs:
- Diffuse redness, hotness & tenderness of the breast (signs of inflammation)
- Enlarged elastic tender lymph nodes.
3. Stage of Acute Abscess
Symptoms:
- Throbbing pain.
- Discharge (pus).
Signs:
- Hectic fever (i.e. at night it may reach 40 degrees or more due to absorption of toxins due to vasodilatation).
- Edema of the overlying skin.
- No response to medical treatment. (Persistence of local signs > 5 days or severe systemic upset > 2 days after full antibiotic treatment).
- Fluctuation is a late sign.
NEVER WAIT FOR FLUCTUATION lN BREAST ABSCESS.
4. Stage of Chronic Abscess
- Attacks of remission and exacerbation
- Tender swelling with yielding center (Paget's Test).
The full details of chronic breast abscess will be discussed separately in another article.
Differential Diagnosis
1. Retro mammary abscess: pain on pushing breast not on bimanual examination.
2. Mastitis carcinomatosis: see the table below.
| Acute Lactational Mastitis | Mastitis Carcinomatosis |
|---|---|
Symptoms:
|
Symptoms:
|
Investigations
It is mainly a clinical diagnosis, but sometimes you may need the following investigations:
- TLC, ESR & CRP: Increased.
- Culture & sensitivity after drainage and to exclude mastitis carcinomatosis.
- Ultrasonography for detection of maturity of pus loculus and its location.
Prevention of Lactational Mastitis (Prophylactic treatment)
a) During last 2 months of pregnancy:
- Massage the nipple if not protruding
- Good hygiene of nipple (Panthinol)
b) After delivery:
- Clean the nipple after suckling by wet tissue (alcohol free)
- If the nipple is fissured >> paint it with antiseptic cream
- If milk engorgement occurs >> Pump evacuation.
Treatment of Lactational Mastitis
1. Before development of an abscess:
Lactation should be stopped from the affected side with treatment according
to stage:
a) Milk engorgement >> evacuate the breast with a breast pump in combination with hot backs
b) Cellulitis >> as before with use of anti staph antibiotics (flucloxacillin or Augmentin @) and
analgesics.
If the child is older than 9 months weaning should be advised.
2. Stage of pyogenic abscess :
Surgical (incision and drainage):
Once pus loculus = drainage
Do not wait for fluctuation (late sign).
Steps of incision and drainage:
a. General anesthesia.
b. Incision:
- Radial incision of the skin, not reaching areola
- if small abscess ) circum-areolar incision may be used for cosmetic
- purpose.
- Counter incision might be needed to leave a drain (if the abscess is large & in a non dependent region).
c. Introduce finger to destroy loculi and send pus for C & S.
d. Antibiotics & postoperative dressing (till healing is complete).
e. Drain is removed when drainage stops.
Some authors advise in cases of early breast abscess, repeated aspiration guided by U/S under antibiotic cover and this often allows resolution without the need for an incision scar and will also allow the patient to carry on breast feeding.
Antibioma: if antibiotic is used in the presence of undrained pus, Antibioma will occur in the form of large sterile brawny edematous swelling that takes many weeks to resolve.
To wean or not to wean
The advisability of weaning is controversial, but a reasonable approach is:
- If the baby is older than 9 months: Stop breast feeding and give Parlodel 2.5 mg twice daily. start with low dose then increase gradually.
- If the baby is younger than 9 months: Continue feeding by the healthy breast and evacuate the diseased breast by a pump.